Hospitals in a time of COVID-19
The experiences of a health professional at a public hospital, March 2020
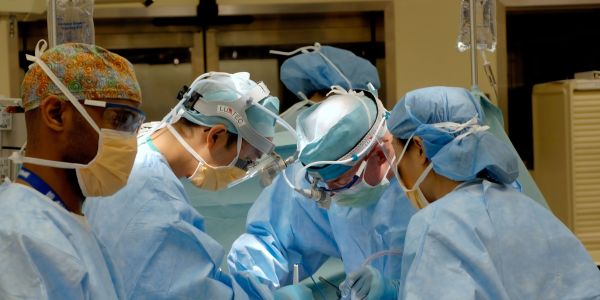
Image: National Cancer Institute - Unsplash
I work in the frontline and am not involved in many of the planning meetings, but I have been told the executives, managers and departmental heads are in COVID meetings all the time. In every meeting or information session that I have personally attended, there is always a disclaimer at the start saying that whatever we were going to be told may be all different by the next day due to the rapidly evolving situation. Hence, employees in the frontline are obliged to read regular updates which can be up to twice daily; this has been going on since January. I also get multiple updates from the department of health, the various professional organisations I am a member of, and media and journal publications which are all coming at an alarming rate.
I can’t tell you how many videos I’ve watched on how to don and doff personal protective equipment (PPE). These are procedures we are familiar with but it is great to have the opportunity to ensure we are doing it right. I am a physician and I have been considering wearing surgical scrubs at work. As it is, it is difficult for older patients to know who is who, soon we will all look the same dressed in surgical scrubs. We have to familiarise ourselves with staff testing criteria and COVID19 case definition criteria which keeps changing!! We have all been assessed on our techniques on how to perform throat and nasopharyngeal swabs. I am personally glad that we are being prepared for what feels like a battle while things are still relatively calm.
Some wards have been recommissioned and furnished in preparation for the event we need extra hospital beds. Extra ICU beds are being set up in pods and portables. Elective surgeries have been scaled back and planned non-elective surgeries have been deferred. The hospital medical records staff and clerical staff are inundated with having to contact people on the waiting list. All visitors to the hospital, including patients and their support persons, are being screened. They will be turned away if they have respiratory symptoms regardless whether it fits COVID criteria if their attendance to the hospital is non-urgent. Clinics have either been cancelled or moved to telemedicine to protect vulnerable patients from possible exposure if they came to hospital. Some staff are really embracing the preparation for the challenge ahead, some are still disbelieving while others look stunned. Right now, the hospitals in our health service have a surreal atmosphere where it is all calm and quiet on the inside with empty beds and empty wards, but chaos in the emergency departments and pop-up fever clinics.
There is a concern that we may have physical beds but may not have enough staff to man them. In addition, it is anticipated that 25% of staff may be away on sick leave during busy times. We have been asked to cancel our annual leave, conference leave and study leave. The health service has not endorsed any overseas travel since late February, and any staff who will have to self-isolate due to unendorsed travel will not be paid. There are strategies to enroll the assistance of St John Ambulance staff and final year students on clinical placements in the event of staff shortages, although these plans have not been widely publicised. Senior registrars will be required to do extra shifts in emergency department regardless of which clinical training programme they are in. Geriatricians whose clinics have been cancelled are being deployed to hospital outreach which services nursing homes. Staff are required to check their temperature daily before going to work.
We have had to change the way we work on the aged care ward. Our multidisciplinary teams are used to working with families of older patients, involving them in their nursing care or in therapy sessions. Multidisciplinary case conferencing, which is one of the hallmark of our type of clinical care, is also problematic with the physical distancing requirement. We cannot hold family meetings, which is another feature of our work, due to restrictions in visitor numbers. By the way, we prefer to use the term physical distancing (and social solidarity) rather than social distancing. Video conferencing from different rooms feel odd. Anyhow, most of our work spaces are hot-desked, so we don’t actually have enough equipment to videoconference. There has also been a new directive that our office spaces will be cleaned daily– hurray! Logistical issues are being revealed every day and I actually feel relieved we are being forced to improve our working spaces.
There is concern that hospitals will soon run out of resources. Locations of hand sanitisers have been moved to areas where they can be under surveillance but may not be in the most practical areas for patient care. PPEs are being rationed to cases where COVID is confirmed or highly suspected, which may be too late if PPEs were not worn for cases with low index of suspicion that are subsequently confirmed to be positive. Staff have been instructed to report any thefts of hospital equipment. Extra security guards have been employed to guard all entrances and exits, and to enforce hand hygiene for everyone entering and leaving hospitals.
In addition, we are starting to see flu cases already. It is unclear if flu season has started early this year or because we are swabbing more people earlier. Flu vaccines won’t be available till late April. Swabs are usually tested not just for COVID but for other respiratory pathogens as well. So the cost of testing will have to take into account the cost of testing for a panel of pathogens, not just COVID. One of the public health messages was for people to have their flu vaccines, in order not to inundate hospital resources with flu also.
I suspect that some of the changes that appear to be made in a hurry have been in the pipeline for some time, but COVID had made them more acceptable. These are telemedicine, and the ability for managers and executives, and administrative staff (clerical) to work from home. I will not be surprised if they become the new normal.
[Source: Clinician, public hospital, Master of Ageing student]